Congenital heart defects
What are congenital heart defects?
Congenital heart defects (congenital vitia) are structural anomalies of the heart that are present at birth. The most common congenital heart defects are, for example, the bicuspid aortic valve, the atrial septal defect or an enlargement of the aorta. Congenital heart defects can be diagnosed during pregnancy, after birth or in adulthood. Not all heart defects require surgical correction; regular observation is often sufficient.
Structure of the heart
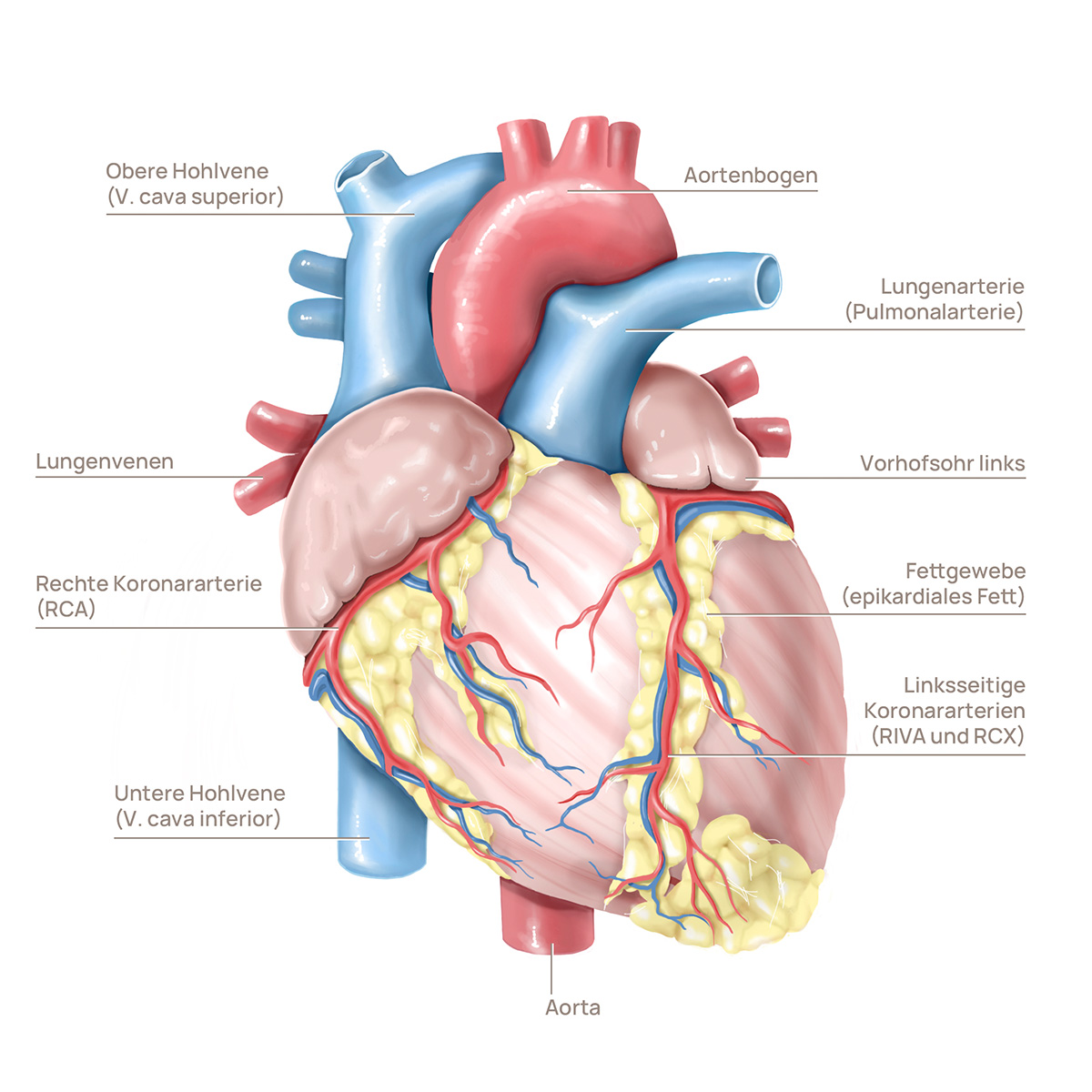
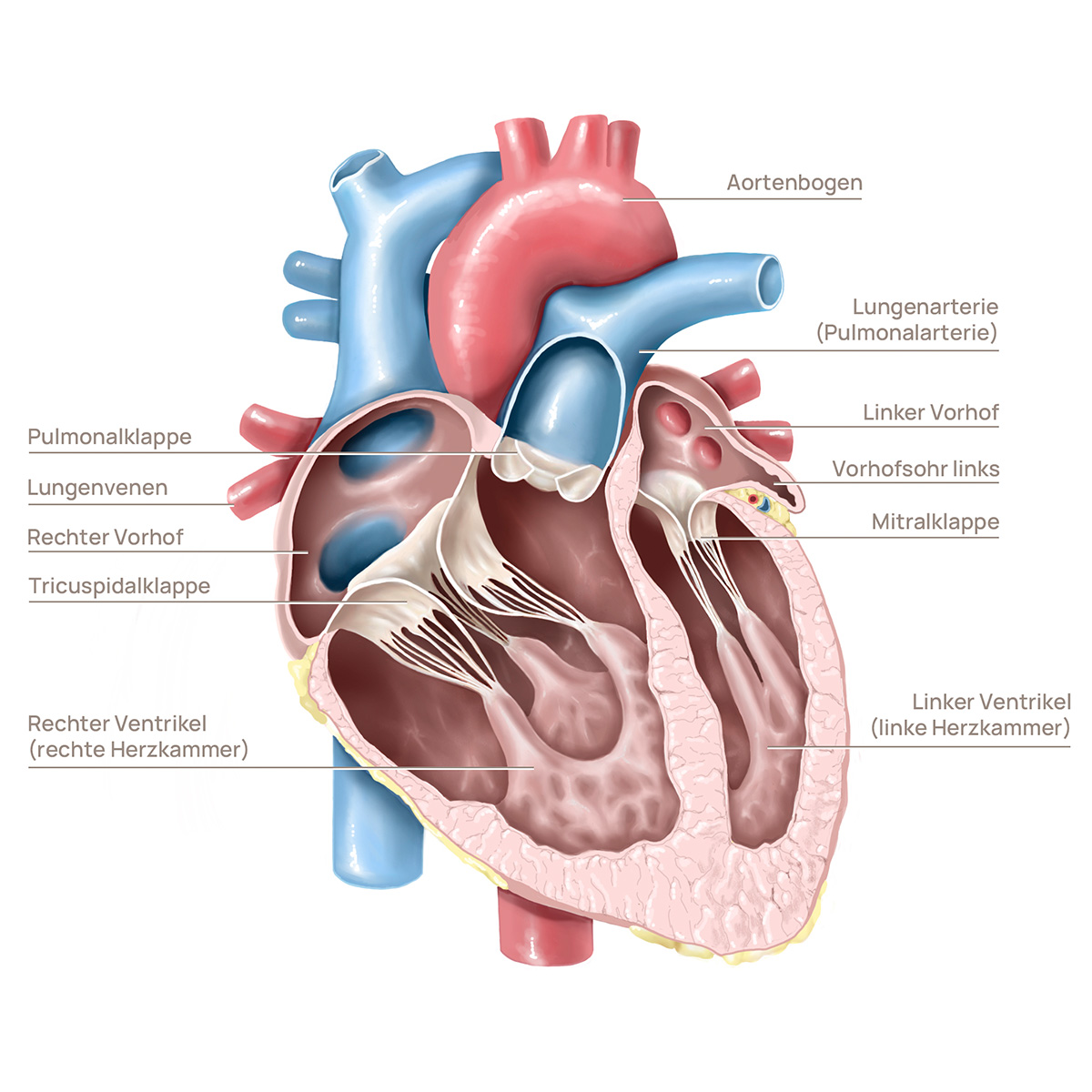
Prevalence and frequency of a congenital heart defect
In Switzerland, around one in a hundred newborns is born with a heart defect. This affects 600 to 800 children every year. These heart defects vary in severity and require different treatment approaches.
Causes and types of congenital heart defects
Heart defects can be caused by various factors:
-
Viral diseases of the mother
-
Use of addictive substances during pregnancy
-
Hereditary diseases
In many cases, the cause remains unknown.
Anatomical categories
Openings in the partitions:
Narrowing of heart vessels (stenosis):
Abnormal position:
Insufficient development:
Symptoms of congenital heart defects
Reduced performance:
Babies sweat profusely when feeding, have difficulty drinking and gain weight slowly.
Blue discoloration:
Cyanosis of the skin and mucous membranes.
Cardiac arrhythmias:
- Breathing difficulties
- Liver enlargement
- Growth disorders
Some heart defects only cause symptoms later in life and remain undetected for a long time.
Differences between childhood and adult heart defects
Diagnosis and treatment
The treatment of heart defects in children differs considerably from that in adults. The European Society of Pediatric Cardiology distinguishes between 2,000 congenital heart defects, which leads to a variety of control and treatment approaches.
Growth-related adjustments
Children with heart defects often require several operations, as prostheses and other therapeutic measures reach their limits as the body grows.
Quality of life and long-term care for a congenital heart defect
Transition to adulthood
Around 90% of affected children reach adulthood. The transition from pediatric cardiology to adult cardiology and taking responsibility for one's own health are decisive phases.
Work and school
Children with heart defects often require several operations, as prostheses and other therapeutic measures reach their limits as the body grows.
Specific heart defects
HLHS is a severe congenital heart defect. The left side of the heart is severely underdeveloped. This means that only the right half of the heart can be used as a pumping chamber.
Newborns quickly show symptoms such as heart failure. The diagnosis is made by echocardiography.
Drug therapy for hypoplastic left heart syndrome
Drug therapy is only part of the treatment plan for HLHS. In the long term, surgical interventions are required to reconstruct the blood flow in the heart.
Interventional therapy for hypoplastic left heart syndrome
Cardiac catheterization to create a left-to-right shunt. A left-to-right shunt is a circulatory disorder in which oxygen-rich blood flows from the arterial part of the circulation (e.g. from the left side of the heart) directly into the venous part of the circulation (e.g. into the right side of the heart).
Surgical therapy for hypoplastic left heart syndrome
In the long term, surgical interventions are required to reconstruct the blood flow in the heart. These interventions typically take place in several stages:
1st Norwood operation:
In the first weeks of life.
2nd Hemi-Fontan or Glenn operation:
At the age of 3-6 months.
3rd Fontan operation:
From the age of 18 months to 3 years.
Tetralogy of Fallot comprises four different heart defects:
1. narrowing of the outflow tract of the right ventricle (pulmonary stenosis):
This narrowing means that the heart has to work harder to pump the blood through the narrowed valve into the lungs.
2. large ventricular septal defect (VSD):
A large ventricular septal defect is a hole in the wall between the left and right ventricles that allows abnormal blood flow between the two chambers.
3. overriding aorta (riding aorta):
The aorta is positioned so that it receives blood from both the right and left ventricle, resulting in a mixture of deoxygenated and oxygenated blood.
4. thickening of the muscle wall of the right ventricle (right ventricular hypertrophy):
A thickening of the muscle wall of the right ventricle as a result of the increased workload caused by pulmonary stenosis.
Symptoms and diagnosis of tetralogy of Fallot
Cyanosis (blue discoloration), heart murmurs and life-threatening seizures are typical. The diagnosis is made by echocardiography.
Treatment for tetralogy of Fallot
An operation, usually at the age of 6-18 months, corrects the malformations. The long-term prognosis depends on the extent of the narrowing.
Therapeutic approaches for heart defects
Treatment methods for heart defects
Drug therapy:
Maintenance of the vascular connections.
Surgical interventions:
Closure of holes, widening of constrictions.
Catheter interventions:
Minimally invasive techniques such as balloon dilatation and umbrella implantation.
Effects on everyday life with a congenital heart defect:
Conclusion on a congenital heart defect
Congenital heart defects are complex diseases that require individual diagnosis and treatment. With modern medical methods, many of those affected can lead a largely normal life. Regular check-ups and close cooperation with specialists are crucial to ensure the best possible quality of life.

